Quality Treatment With Super Affordable Price


- goldmedalphysiotherapy@gmail.com
- 45, Eros City Square Mall, Sector 49, Gurugram
Call us anytime
Best Physiotherapy Treatment India
Call us anytime
Write a mail
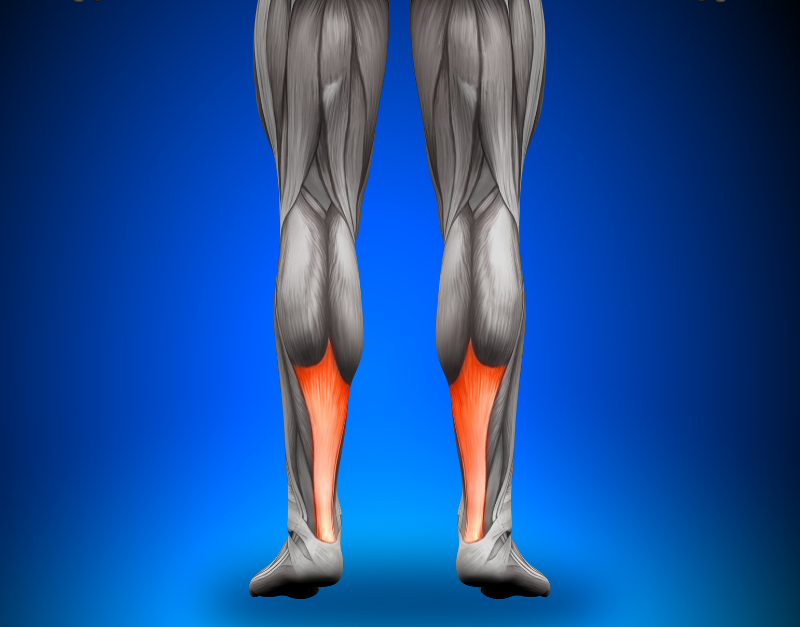
The Achilles tendon, a vital band of tissues linking the calf muscle to the heel bone, is essential for walking and elevation. However, when stretched past its limitations, this tendon is prone to rupture, partly or totally. In this blog article, we’ll look at the signs, symptoms, causes, diagnosis, and treatment options for Achilles tendon rupture, including surgery and non-surgical treatments, as well as the critical function of physiotherapy in the rehabilitation process.
Achilles tendon rupture causes severe agony, a perceptible crack or snap sound, swelling behind the heel, and the inability to elevate the heel. A complete physical examination is performed, including specialised tests such as the Thompson Test and Matles Test and imaging modalities such as X-ray, ultrasound, and MRI.
This injury is most prevalent within 6 cm of the tendon’s connection to the heel bone, a location with inadequate blood supply. Common causes include forceful leaping, abrupt running accelerations, falls, and tripping. Middle-aged people who participate in sports like leaping and running are especially vulnerable to Achilles tendon rupture.
To confirm an Achilles tendon rupture, doctors use various diagnostic methods. A thorough evaluation includes the Thompson Test, Matles Test, ATR-score questionnaire, real-time Achilles ultrasonography Thompson test, X-ray, ultrasound, and MRI. These techniques help to determine the degree of the rupture and detect any underlying tendon diseases.
The decision between surgery and non-surgical therapy is influenced by age, activity level, and injury severity. The ruptured tendons are stitched together and occasionally strengthened with extra tendons after surgery. Non-surgical techniques include immobilisation using boots or casts, as well as medicine such as NSAIDs and pain relievers. Patient education is critical, emphasising the necessity of following recommended therapies and refraining from activities that cause discomfort or oedema.
Physiotherapy in affordable price is critical in the recovery from Achilles tendon rupture. Immobilisation using boots or casts, cryotherapy to minimise inflammation, ultrasound treatment for early healing, and transcutaneous electrical stimulations (TENS) for efficient suture healing are all components of physiotherapy.
A complete physiotherapy regimen includes a range of motion exercises, flexibility exercises, gradual ankle strengthening, balance and proprioception exercises, plyometrics, and aerobic conditioning. These exercises are designed to assist patients in reestablishing standard movement patterns by restoring strength, flexibility, and function to the damaged region.
Patient education is a critical component of Achilles tendon rupture treatment. Patients are advised to avoid painful or swollen workouts and maintain strength and stability exercises even after recovering. Some concerns may last up to a year, and a gradual reintroduction to high-level activity is suggested for best results.
Achilles tendon rupture is a problematic condition that needs thorough evaluation and treatment. Physiotherapy is essential for a good recovery, whether surgical or non-surgical therapies are used. Patients can actively engage in rehabilitation by knowing the origins, symptoms, and treatment choices, working towards recovering strength, stability, and functionality in the afflicted region. Remember that patience and consistency are essential to rehabilitation, leading to a triumphant return to regular activities.
Gold Medal Physiotherapy is a shining example of thorough Achilles tendon rupture treatment. Gold Medal Physiotherapy assures a gold standard in recovery and rehabilitation by having a complete awareness of the injury’s origins, symptoms, and treatment choices, as well as an emphasis on patient education and personalised physiotherapy regimens.
Achilles tendon ruptures are frequently caused by violent leaping, rapid accelerations in running, and activities such as tripping or falling.
A complete physical examination, including tests such as the Thompson Test and Matles Test and imaging modalities such as X-ray, ultrasound, and MRI, is required for diagnosis.
Treatment options vary depending on characteristics such as age and severity of the injury, ranging from surgery, which involves tendon sewing, to non-surgical procedures such as immobilisation and medicines.
Physiotherapy, which includes a range of motion exercises, flexibility training, gradual ankle strengthening, balancing activities, plyometrics, and aerobic conditioning to restore strength, flexibility, and function, is critical in recovery.


Quality Treatment With Super Affordable Price
Call us anytime
